- By Tagore Admin
- Posted June 22, 2023
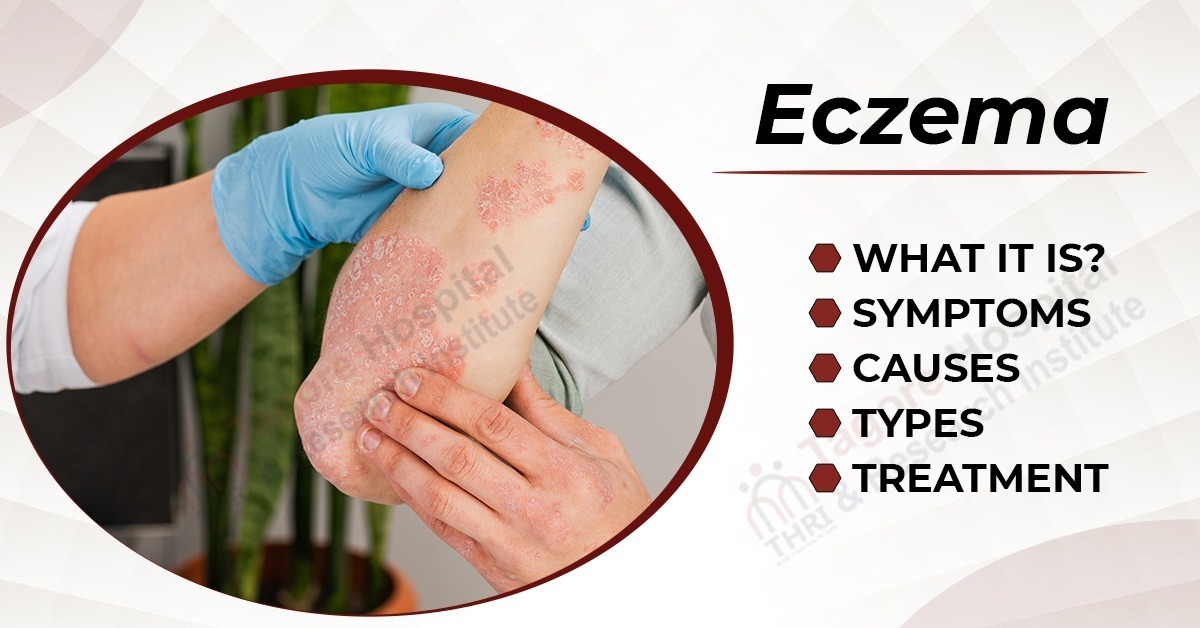
What is Eczema?
People of all ages are susceptible to the chronic inflammatory skin condition known as eczema, also known as atopic dermatitis. It is characterized by skin patches that are red, itchy, and inflamed. Eczema is thought to have a genetic and environmental component, though the exact cause is unknown.
The primary symptom of eczema is a compromised function of the skin barrier. The skin typically serves as a barrier, stopping moisture loss and protecting the body from irritants and allergens. This barrier function is impaired in people with eczema, making the skin more prone to dryness, itching, and sensitivity.
Types of Eczema
There are several types of it, each with its characteristics and triggers. The most common types of eczema include:
1. Atopic Dermatitis: This is the most prevalent form of eczema and often appears in infancy or early childhood. It is characterized by redness, inflammation, and dry, itchy skin. Atopic dermatitis is associated with a family history of allergic conditions like asthma and hay fever.
2. Contact Dermatitis: Whenever the skin comes into contact with an allergen or irritant, contact dermatitis develops. Contact dermatitis can take one of two forms:
a. Allergic Contact Dermatitis: It develops when the immune system reacts to a specific allergen, such as certain metals, latex, or certain chemicals.
b. Irritant Contact Dermatitis: This occurs when the skin is exposed to irritating substances like detergents, solvents, or cleaning products. More people experience irritant contact dermatitis than allergic contact dermatitis.
3. Nummular Dermatitis: This type of eczema is characterized by circular or coin-shaped patches of irritated skin that are usually itchy and can be quite persistent. It often occurs on the arms, legs, or torso and can be triggered by dry skin, stress, or environmental factors.
4. Seborrheic Dermatitis: Seborrheic dermatitis primarily affects the scalp, face, and other areas with a high density of oil glands. It causes redness, scaling, and dandruff-like flakes. In infants, it is commonly referred to as "cradle cap."
5. Dyshidrotic Eczema: Dyshidrotic eczema is characterized by small, itchy blisters that appear on the hands and feet. These blisters may be accompanied by redness and flaking. The cause of dyshidrotic eczema is unknown, but it is believed to be associated with allergies, stress, or exposure to certain metals.
6. Stasis Dermatitis: Stasis dermatitis typically occurs in the lower legs and is associated with poor circulation in the veins. It is often seen in individuals with varicose veins or venous insufficiency. Symptoms include redness, itching, and swelling.
Read also: Heart Disease: Symptoms, Causes, Risk Factors, Prevention, And Treatment
Causes of Eczema
Although the precise causes of eczema are not fully understood, it is thought that a combination of genetic, immune system, and environmental factors contribute to the condition. Several things can cause eczema to manifest itself, including the following:
1. Genetic predisposition: Eczema frequently runs in families, pointing to a hereditary basis. Certain variations in genes can affect the skin's barrier function, making it more susceptible to moisture loss and external irritants.
2. Immune system dysfunction: People with eczema tend to have an overactive immune system that reacts excessively to triggers, leading to inflammation and skin irritation. This immune dysfunction is associated with an abnormal response to allergens and irritants.
3. Skin barrier defects: The skin acts as a protective barrier that helps retain moisture and keep out harmful substances. In eczema, the skin barrier is impaired, allowing moisture to escape and irritants to penetrate more easily. This makes the skin dry, itchy, and prone to inflammation.
4. Allergies: Allergies, such as food allergies or allergic rhinitis (hay fever), can contribute to eczema in some individuals. Exposure to allergens can trigger an immune response, leading to eczema flare-ups.
5. Environmental factors: Various environmental factors can worsen eczema symptoms or trigger flare-ups. These include dry climates, hot or cold temperatures, low humidity, exposure to certain irritants (like harsh soaps or detergents), and contact with allergens such as pollen, dust mites, pet dander, or mold.
6. Stress: Emotional stress can exacerbate eczema symptoms. Stress triggers certain physiological responses in the body that can affect the immune system and increase inflammation, potentially worsening eczema.
7. Hormonal changes: Changes in hormone levels, especially in women, might affect eczema symptoms. Eczema may worsen during pregnancy or at certain stages of the menstrual cycle.
It's important to note that triggers and causes can vary from person to person, and identifying individual triggers can help manage and prevent eczema flare-ups.
You Can Read Also:- Facts You Need To Know About Blood Cancer (Leukemia)
Symptoms of Eczema
The symptoms of eczema can vary in intensity and appearance from person to person, but they generally involve the skin becoming dry, itchy, and inflamed. Here are the common symptoms associated with eczema:
1. Dry skin: Eczema often causes the affected skin to become excessively dry, rough, and scaly. It may appear flaky or feel rough to the touch.
2. Itching: The defining symptom of eczema is itching, which is typically severe. The urge to scratch the affected areas can be overwhelming, and scratching can worsen the condition, leading to further inflammation and potential skin damage.
3. Redness and inflammation: The skin affected by eczema often becomes red, inflamed, and irritated. This can be more noticeable during eczema flare-ups.
4. Rash or patches: Eczema typically presents as patches of skin that are red, and raised, and may develop a rough or leathery texture. The affected areas can vary in size and shape, and they may be accompanied by small bumps or blisters.
5. Swelling: Inflammation caused by eczema can lead to swelling, particularly in severe cases or during flare-ups. Swollen skin may feel tender or warm to the touch.
6. Cracking or oozing: In some instances, eczema can cause the skin to crack or split. Additionally, if the affected skin becomes severely inflamed, it may ooze fluid or develop crusts.
7. Thickened skin: Over time, frequent scratching and rubbing of the affected areas can lead to the skin becoming thickened and developing a leathery texture. This is known as lichenification and is commonly seen in chronic or long-standing cases of eczema.
Treatment of Eczema
The treatment of eczema aims to manage symptoms, relieve itching, reduce inflammation, and improve skin barrier function. The specific treatment approach may vary depending on the severity of the condition and individual factors. Here are common treatment options for eczema:
1. Moisturizers: Regular and frequent application of moisturizers helps to hydrate the skin and restore its barrier function. Look for thick, fragrance-free creams or ointments that lock in moisture. Apply moisturizer after bathing or showering to seal in hydration.
2. Topical corticosteroids: A healthcare provider may advise the use of these anti-inflammatory creams or ointments. They help reduce inflammation and relieve itching during eczema flare-ups. Corticosteroids come in different strengths, and the appropriate strength and duration of use should be determined by a healthcare professional.
3. Topical Calcineurin Inhibitors: These medications, such as tacrolimus or pimecrolimus, also help reduce inflammation and are particularly useful for sensitive areas like the face and groin. They are often recommended when corticosteroids are not suitable for long-term management.
4. Topical Phosphodiesterase-4 (PDE4) Inhibitors: Crisaborole is a nonsteroidal topical ointment that inhibits PDE4 enzymes, reducing inflammation and symptoms of eczema. It is prescribed for mild to moderate cases of eczema in patients aged 2 years and older.
5. Antihistamines: Oral antihistamines can help relieve itching and aid in better sleep during eczema flare-ups. They may cause drowsiness, so it's important to follow the recommended dosage and consult with a healthcare professional.
6. Wet Wrap Therapy: This involves applying a moisturizer to the affected areas and then covering them with wet bandages or clothing. Wet wrap therapy helps to enhance moisturization, soothe the skin, and reduce itching.
7. Avoiding Triggers: Identifying and avoiding triggers that worsen eczema symptoms is important for managing the condition. Common triggers include certain soaps or detergents, harsh fabrics, allergens, extreme temperatures, and stress. Keeping a journal can help identify specific triggers.
8. Other Medications: In severe cases of eczema that do not respond to other treatments, systemic medications may be prescribed. These include oral corticosteroids, immunosuppressants, or biologic drugs. These drugs should only be taken as prescribed by a healthcare professional due to the possibility of side effects.
9. Behavioral Therapies: Stress management techniques, such as relaxation exercises, meditation, and counseling, can help reduce stress and improve eczema symptoms in some individuals.
Prevention of Eczema
While it may not be possible to completely prevent eczema, there are measures you can take to minimize flare-ups and reduce the severity of symptoms. Here are some prevention strategies for eczema:
1. Moisturize regularly: Keeping the skin well-hydrated is crucial in preventing eczema flare-ups. Apply moisturizers or emollients daily, especially after bathing or showering, to lock in moisture and maintain a healthy skin barrier.
2. Avoid irritants: Identify and avoid substances that can irritate your skin or trigger eczema symptoms. These can include harsh soaps, detergents, fragrances, certain fabrics (like wool), and chemicals. Opt for gentle, fragrance-free skin care products and laundry detergents that are suitable for sensitive skin.
3. Choose gentle cleansers: Use mild, non-irritating cleansers when bathing or washing your hands. Avoid hot water, which can strip the skin of natural oils, and opt for lukewarm water instead. Instead of rubbing, gently pat your skin dry with a soft towel.
4. Moisturize after water exposure: After swimming or prolonged water exposure, moisturize your skin to replenish lost moisture. Those with sensitive skin should pay special attention to this.
5. Identify and manage triggers: Keep track of factors that seem to trigger your eczema flare-ups, such as specific foods, allergens, stress, or environmental conditions. Taking steps to minimize exposure to these triggers can help prevent or reduce the frequency and severity of flare-ups.
6. Dress in soft, breathable fabrics: Choose clothing made from soft, natural fibers like cotton or silk. Avoid rough, scratchy materials that can irritate the skin, such as wool or synthetic fabrics.
7. Maintain a consistent temperature and humidity: Extreme temperatures and low humidity levels can aggravate eczema. Keep indoor environments comfortable and use a humidifier during dry seasons to add moisture to the air.
8. Manage stress: Stress can exacerbate eczema symptoms in some individuals. Practice stress management techniques such as relaxation exercises, meditation, or engaging in activities that help you unwind.
9. Protect your skin: Shield your skin from harsh weather conditions, such as cold winds or excessive sun exposure. Wear appropriate clothing, use sunscreen, and apply a barrier cream before coming into contact with irritants or allergens.
10. Seek medical advice: If your child has eczema, consult a healthcare professional, such as a dermatologist. They can provide guidance, prescribe suitable medications if needed, and help develop a personalized management plan.
Summary
Eczema, also known as dermatitis, is a common skin condition characterized by dry, itchy, and inflamed skin. It can be chronic and recurrent, causing discomfort and impacting the quality of life. Eczema is thought to be caused by a confluence of genetic, immune system, and environmental factors, though its exact cause is still unknown.
To prevent eczema flare-ups and reduce symptoms, several measures can be taken. Moisturizing the skin regularly with gentle, fragrance-free moisturizers helps to maintain the skin's hydration and strengthen its protective barrier. It is important to avoid irritants such as harsh soaps, detergents, and certain fabrics that can trigger or worsen eczema. Opting for mild cleansers, avoiding hot water, and patting the skin dry gently after bathing are recommended.
Identifying and managing triggers specific to individuals, such as certain foods, allergens, stress, or environmental conditions, can significantly help prevent eczema flare-ups. Wearing soft, breathable fabrics and protecting the skin from extreme weather conditions also play a role in prevention. Stress management techniques, including relaxation exercises and meditation, can be beneficial, as stress can exacerbate eczema symptoms.
While it may not be possible to completely prevent eczema, following these prevention strategies can minimize flare-ups, reduce the severity of symptoms, and improve the overall health of the skin. It is important to consult with a healthcare professional, such as a dermatologist, for an accurate diagnosis, personalized advice, and appropriate treatment if necessary.
Tags